
Traumatic Births: “A Club No One Wants to Join”
By Lizzie Marvelly
Lizzie Marvelly (Ngāti Whakaue) wasn’t afraid of giving birth — she felt well prepared and with realistic expectations about what lay ahead. But her experience in a main centre public hospital left her physically and emotionally battered. She tells her story here. Additional reporting on the state of maternity care by Ollie Neas.
* Some names have been changed.
Sweltering in the blistering heat of December, I couldn’t wait to go into labour. I read all the old wives’ tales, ate all the medjool dates, walked countless kilometres through the Rotorua Redwoods and . . . nothing. I’ve since learnt that my baby has a determined streak and follows her own schedule. She wasn’t coming until she was good and ready.
My waters finally broke at 40 long weeks and three days, at 9:15pm on 17 January. I was thrilled — mildly apprehensive about what lay ahead, but excited. I was about to meet our precious baby. I had a birth plan and felt confident that I would approach the challenge of labour with strength and fortitude. Women have been giving birth for millennia — in caves, in hospitals, at home. I would too.
What I couldn’t have predicted was that I’d still be enormously pregnant two days later, and in the midst of the most terrifying experience of my life. As my GP would later say, had I given birth 100 years ago, it’s likely my baby and I would’ve died. As it was, in 2022, in Rotorua’s large regional hospital, my wife worried that she would lose us both.
You don’t hear much about birth trauma until you’ve experienced it yourself, then all of a sudden, women you’ve known for both minutes and years open up about the horrendous things that happened to them. Some are too terrified to have another child. Some have suffered crippling post-partum depression and post-traumatic stress disorder. Some can’t even use a tampon without experiencing a visceral reaction.
Once you’ve lived through a traumatic birth you become a member of a club no one wants to join. You suffer in silence while people wax lyrical about how magical motherhood is and how much you must love being a mum. You’re served Instagram ads about memorialising your birth story while you cry quietly in the dead of the night feeding your tiny newborn, grieving for the birth experience you wish you’d had.
Mostly, women keep this trauma to themselves. But I’ve never been great at silence. Six weeks after my daughter was born, I penned a social media post in the early hours of the morning — sitting in the darkness, tapping away at my phone, with tears streaming down my face. Until that point I hadn’t been able to talk about my birth story without experiencing intense, terrifying flashbacks. Reliving it this time felt different. Though I didn’t register it at the time, I was taking back my agency over something that rendered me completely powerless.
It may seem odd to speak of power and agency in relation to birth — a primal process in which one’s body largely takes over — but there is a chasm between willingly giving in to your body’s natural and functional urges and being denied the assistance and support you need as you navigate one of the most vulnerable of life’s experiences.
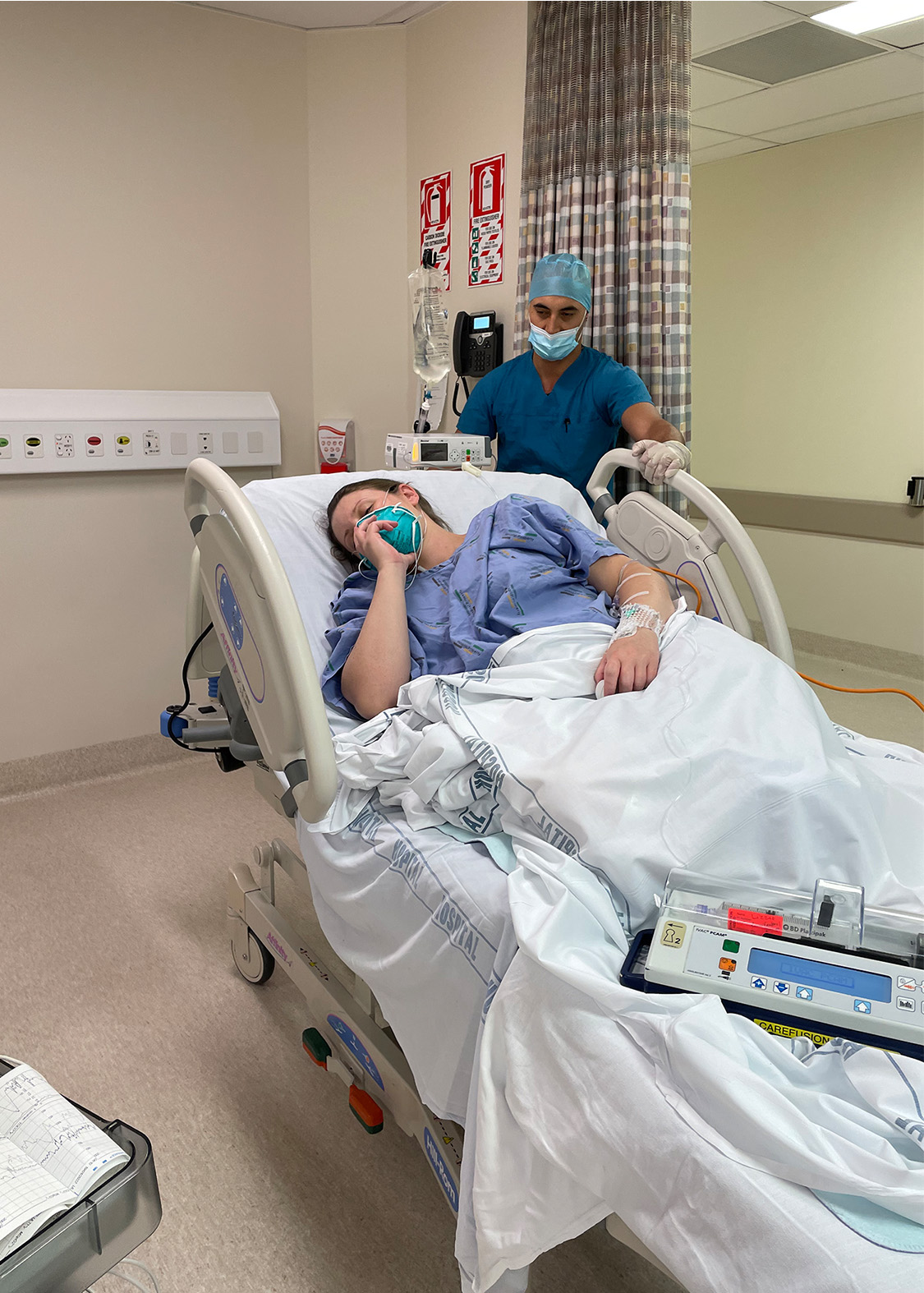
The morning after my waters broke, bleary-eyed after a night of very little sleep, I was experiencing mild and intermittent cramping but nothing else. The contractions I’d been expecting hadn’t started. There’s a 24-hour window after the rupturing of the membranes (the waters breaking) in which a baby should be born – without the protective barrier, bacteria can cause infection. It seemed unlikely that our little darling was going to meet that deadline, so medical intervention was the logical next step. Our midwife Sarah* asked us to go to the hospital to meet with the doctors.
We arrived at Rotorua Hospital shortly after 9am, and met with the duty obstetrician shortly after. After an internal exam it was suggested that the best course of action would be to use a Syntocinon drip to induce contractions. I had always been frightened of an induction because artificially inducing or augmenting labour can cause harder, faster and more painful contractions (and increases the risk of other interventions being needed), but agreed on the basis that I’d be able to receive an epidural if the pain became too intense.
At Rotorua Hospital, epidurals aren’t easy to come by. In the 1990s, a shortage of anaesthetists meant that birthing parents weren’t able to access an epidural at all. Today, an epidural is still not a guarantee, and induction can speed things up to the point where it is not possible to administer one in any case. It was agreed that I could access one — provided an anaesthetist was available. The likelihood of an anaesthetist being free was much higher during the day, so it was decided that the hospital midwives would start the Syntocinon drip as quickly as possible that morning.
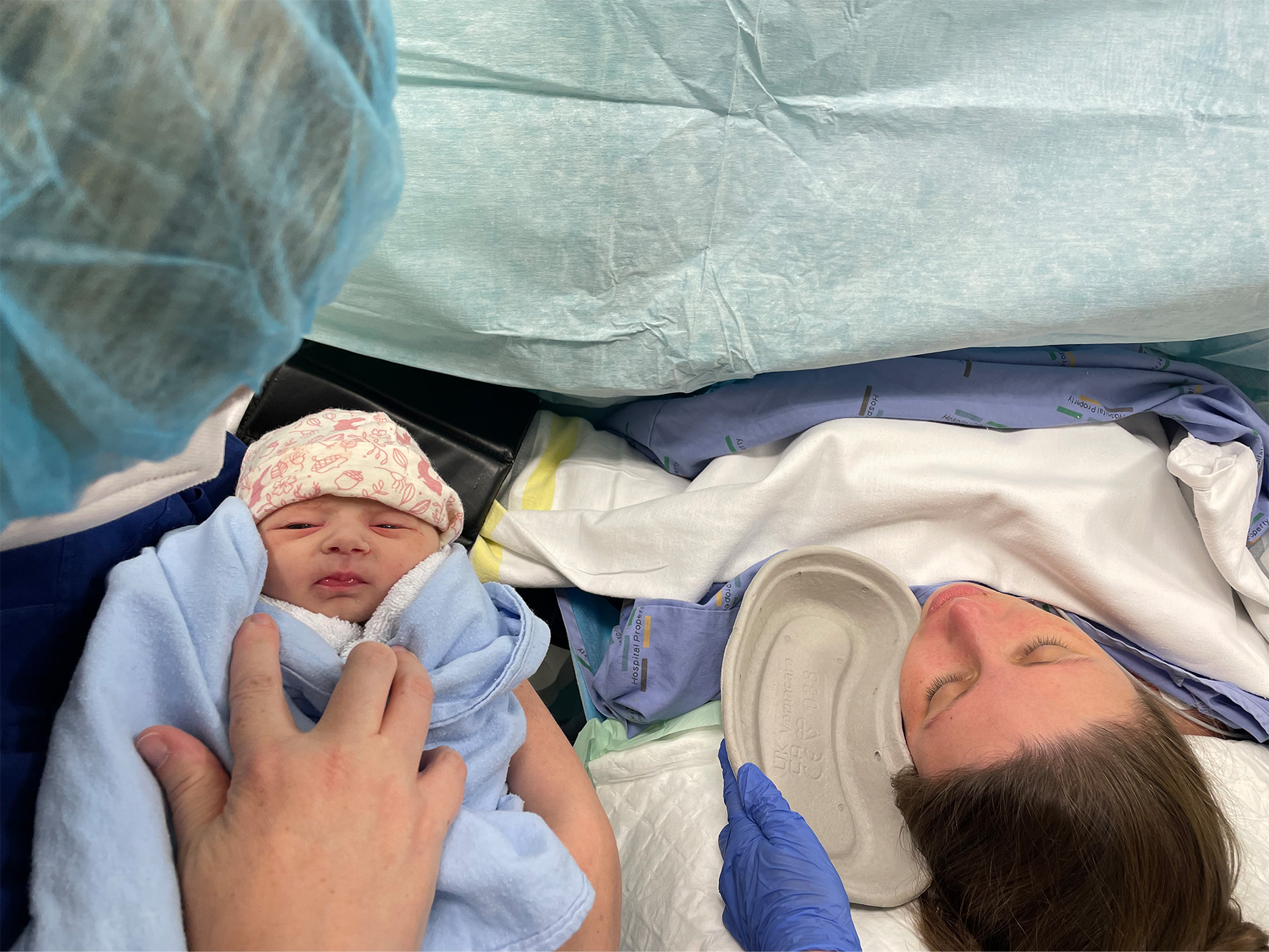
Lizzie and daughter, Ellis Atiraira, born on 19 January at Rotorua Hospital. Photo: Lizzie Marvelly.
An hour went by. Two hours. Four hours. Still no Syntocinon. It was about 2pm when we finally found out that the hospital was short-staffed and the midwives wouldn’t be able to supervise the induction. By this time, it had been nearly 18 hours since my waters broke. My wife Lisa and I were running on about four hours’ sleep.
The solution suggested by the hospital was to ask Sarah to come in and provide the required supervision. Sarah had been up since early that morning, and working with other parents all day. Starting an induction at 3pm would’ve required her to work late into the night. Given how long labour can take, she’d likely have to hand over to another midwife at the point that I most needed her. (She would also be overseeing the induction for free — lead maternity carer (LMC) midwives are not paid to provide this early labour service.) There was no safe option, and I was told by the hospital that I would have to wait until the next morning to be induced. Oh, and after an injection of antibiotics to try to prevent a uterine infection, I could go home if I wanted.
There was no way I was leaving that hospital. About 5pm, 20 hours since my waters broke and still without being induced, I began to feel niggling cramps. They came in waves, and by 8pm they’d turned into mild contractions. Although I was exhausted, I felt excited. Finally, my body had kicked into gear. I could handle another late night, I thought, if it meant we’d have a baby in the morning. How naive I was.
At 9pm, Lizzie and Lisa were advised there would likely be hours of labour ahead. A warm shower was suggested. Lizzie’s contractions continued, but another internal examination at 11pm showed she was only 2 centimetres dilated. They were told by a hospital midwife that Sarah wouldn’t be called in until she got to 5 centimetres, “because she’d be annoyed” to be contacted. Around midnight, Lizzie was in intense pain and the contractions were closer together. Entonox gas was delivered but didn’t do much other than make her light-headed. Remifentanil, a short-acting opioid pain reliever, was requested, but the hospital midwife demurred, and also turned down a request for an epidural, instead suggesting a one-off dose of morphine would help her sleep while dilation continued.
I had major reservations about taking morphine, but as it was the only thing on offer and I was becoming increasingly desperate, I agreed. It was administered in 2 millilitre increments. The hospital midwife suggested that after 4 millilitres I’d likely be asleep. Four millilitres came and went. Six. Eight. I felt woozy and stoned, but the morphine didn’t even begin to touch the pain of the contractions. Instead I felt as if I was in an excruciating, lucid dream, but I was nowhere near sleep. Even the midwife seemed stumped.
It was around this time that I began to implode. I was in increasing agony, utterly exhausted, and felt totally disempowered. My poor wife, who’d been advocating on my behalf for hours, decided that enough was enough, and called Sarah in tears. It was nearly 2am. Without hesitating, she jumped straight in the car, driving for nearly an hour to join us at the hospital by 3am.
Sarah quickly appraised the scene and took control. I needed better pain relief immediately, while we came up with a new game plan.
She performed another vaginal examination and reported that I had made it to just 3 centimetres’ dilation. Remifentanil was finally administered, but it offered no relief other than making me pass in and out of consciousness between contractions. It was better than nothing, however. My contractions were crashing on top of each other with ferocious intensity and achieving very little: I needed an epidural to have a chance to withstand the pain long enough to enable me to fully dilate. When you need an epidural at 3:30am at Rotorua Hospital, however, you may as well write a letter to Santa. Though Sarah did her best to advocate for me, no anaesthetists were answering their pagers, and all of the doctors were engaged elsewhere.
So we waited. And waited. This stretch of time is a blur, but I now know that my wife had been watching the monitor alongside our midwife. My resting heart rate sat at more than 140 beats per minute, as if I was on a treadmill. Our baby’s heart rate began to decelerate. At this stage my waters had broken more than 30 hours ago. I was shivering, vomiting and dehydrated, dissociating to escape the pain and the terror. Lisa was beside herself, watching me writhing in unbearable pain with no end in sight. Terrified, she asked our midwife, “What would have to happen for us to see the doctors?”
When you need an epidural at 3:30am at Rotorua Hospital, you may as well write a letter to Santa.
Throughout my pregnancy, I’d been adamant that I wanted to give birth to our daughter vaginally. It’s the ‘natural’ way, women are told. In antenatal classes, the benefits of vaginal birth are extolled, and caesarean sections are usually only mentioned in passing. But as I approached my 20th hour in hospital, it slowly dawned on me that I had nothing left to give. Even if I had been 10 centimetres dilated, there’s no way I’d have had the energy to push. Sarah asked us which we’d like her to agitate for: an epidural or a caesarean? I felt utterly defeated, but resolute. I needed surgical intervention.
Sarah was finally able to make contact with the doctors at 5:30am. A doctor approved the caesarean shortly after, but there was a shift change about to happen, so we’d have to wait. For another hour I writhed in pain, before suddenly at 7:30am, a troupe of people converged upon our room. By this time I was conscious but barely aware of what was happening around me. What had begun a few hours earlier as gentle shivering had turned into intense, uncontrollable shaking.
As we waited to go into theatre, the surgeons, theatre nurses and anaesthetist visited. I decided to stop the remifentanil so I could attempt to understand what was being said. I barely remember meeting the surgeons, but I remember a comically frightening conversation with the anaesthetist. He told me he’d do something and I’d have to respond in some way to tell him what I could feel. I wasn’t sure what he meant but, too exhausted to ask for clarification, I simply nodded.
I took the same approach to the protracted process of giving consent for the surgical procedure, nodding like a bobble-headed dog on a car dashboard. I knew I was in no fit state to give informed consent. I could’ve been signing away the ownership of my worldly possessions, for all I knew. All I wanted was for the pain to end.
My next memory is of sitting on the theatre bed, hunched over as the anaesthetist attempted to insert the spinal block. “Keep still,” he told me, as I shuddered uncontrollably. No matter what I tried, I couldn’t stop shaking as contraction after contraction crashed through me. I vividly remember the terror of thinking that he would paralyse me because I couldn’t keep still. I would flash back to this moment over and over again in the weeks after the birth.
Finally, he managed to insert the block and I was laid back on the surgical table. The anaesthetist tried to insert an intravenous line into my arm, failing twice because I was so dehydrated.
My overwhelming memories of the actual birth of my baby are of vomiting and shaking continuously. And, like a bright light in the deepest darkness, the cries of our beautiful daughter as she took her first breaths. Thank God. Tihei mauri ora.
Ellis, our much-wanted, much-loved daughter, was dangled above me, then whisked away to be checked. Thankfully, she was fine, although smaller than expected. A key part of my birth plan was for Ellis to be laid on my chest for skin-to-skin contact, and then to initiate early breastfeeding. Neither of those things happened. By this stage I was shaking so hard I was almost convulsing, with tremors that wouldn’t stop for another hour and a half, no matter what the nurses in the recovery area did. I was so exhausted, I was barely conscious. So traumatised I wanted to black out and sleep for a year. I was, as I wrote later on social media, utterly fucking beside myself.
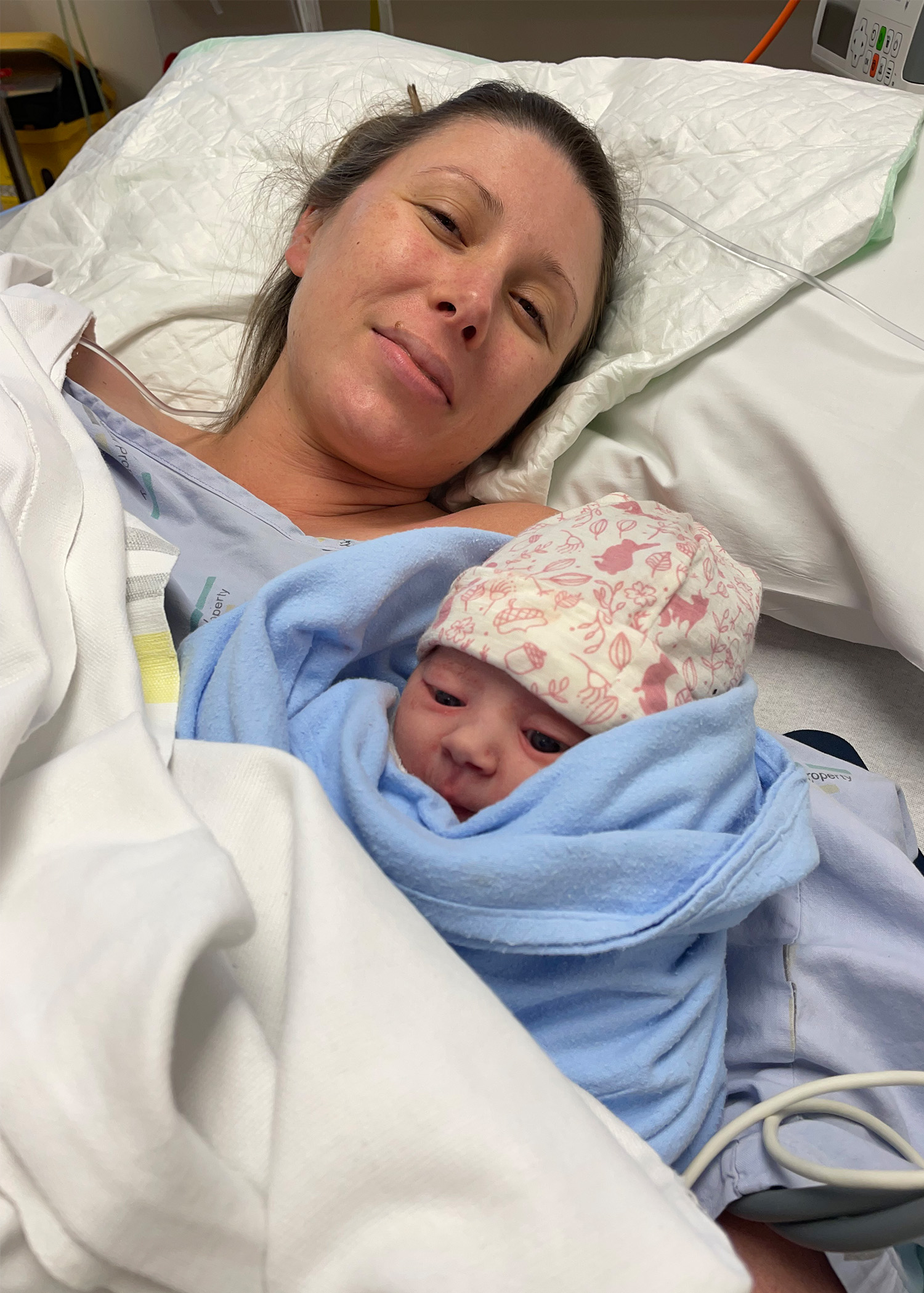
My wife, my daughter and I had a terrifying start, and we all deserved better. In the days that followed, one of the doctors visited my room on the ward and apologised. I felt sympathy for her. It must be awful knowing that you are failing your patients, and you are powerless to do anything about it. With the exception of one dismissive, gatekeeping hospital midwife, all of the other medical staff did their best. Sarah particularly went above and beyond.
My experience was likely avoidable. We were failed by a health system that is chronically underfunded and short-staffed. Of course, there are no guarantees it would have been plain sailing had I been induced, but it was the unavailability of supervision from the hospital midwives that delayed my planned induction. Had I been induced at 10am on 18 January as originally planned, I believe my birth story would’ve been markedly different. The hell and horror I experienced in the dead of the night wouldn’t have happened.
The hospital’s short-staffing went well beyond the birthing unit. In the four days after our daughter’s arrival, there were only two shifts in which midwives were on duty in the maternity unit. The rest of the time, there were only nurses (who were doing their best, but midwives are essential in maternity settings). One afternoon the unit was so short-handed that they had to bring in emergency department nurses to fill the gaps.
A month after Ellis’s birth, I read in the local paper that new mums and babies were being shipped out to general wards, because the Lakes District Health Board couldn’t safely staff the maternity unit. This came after another news story published the day after Ellis was born, in which an unnamed Rotorua midwife claimed that the staffing levels at Rotorua Hospital’s maternity unit were “incredibly unsafe” and “dangerous”. I couldn’t agree more.
(Lizzie’s story and the stories of other mothers continues below)
Risky Business
Understaffed and under equipped maternity wards are pushing midwives to breaking point — and putting women and babies at risk at the moment they most need care.
By Ollie Neas
Every year some 60,000 babies are born in New Zealand. The vast majority are born healthy — but for a small number, it’s a different story. More than 400 babies die each year from birth-related complications, and around 70 more are born with neonatal encephalopathy — a kind of brain damage in newborns, caused mainly by a lack of oxygen.
We all know the headlines: Understaffed maternity wards. Outdated equipment. Midwives pushed to breaking point. In a quarter of birth-related deaths, barriers to access, or personnel or organisational issues were contributing factors. In 2018 alone (the most recent figures available), 79 deaths were classed as potentially avoidable, and in the same year at least three major hospitals had been reporting unsafe staffing levels for more than a year. Between 2014 and 2018, poor management, barriers to care and personnel issues — such as a failure to communicate between staff and lack of skills — were the main contributory factor in 48 potentially avoidable deaths caused by lack of oxygen to the brain during birth over that period. Another study found that around half of moderate to severe neonatal encephalopathy cases are potentially avoidable. Early last year maternity services at Wellington Hospital reached capacity three times, meaning it could not look after any more women.
And while maternal deaths during or shortly after childbirth have been trending down for the last 15 years, in 2020 four women at Auckland Hospital alone died in two months, a cluster which, while unusual, was found in a review to be a result of systemic problems including staff feeling overworked and unsupported, the Weekend Herald reported in an investigation into the deaths. Midwife shortages were found to be having a “significant impact”, the review found.
Birth may be a risky business — a change to the way ACC claims are assessed made by the government late last year acknowledges that up to 18,000 women a year need support for birth injuries ranging from moderate to debilitating — but it doesn’t need to be this risky.
“All of us in the sector have been saying for a long time, ‘We’ve got a problem, we’ve got a problem, we’ve got a problem’,” says Alison Eddy, the chief executive of the New Zealand College of Midwives. “Now the problem is here and it’s not getting any better.”
There are around 3200 midwives licensed to work in New Zealand, though some may not be currently or fully employed. The number of actual working midwives, however, by the District Health Boards’ own staffing calculations, is not enough. For years, midwives have been a feature on Immigration New Zealand’s regional skills shortage list — as at August last year, DHBs nationwide were short nearly 300 midwives, an increase of 89 vacancies since December 2020. Southern DHB has the fewest midwives per 100,000 people.
A leading maternity advocate describes the workforce as a “leaky boat”. “It might feel like you’re pouring water into the top, but it’s leaking out the bottom at the same time.”
While workforce surveys show the total number of working midwives to be fairly static, fewer midwives work full-time than any other DHB workforce, and Eddy says it’s common for midwives to reduce their hours in order to manage the stress of the job — or they leave the profession altogether. “Many of the DHBs simply cannot recruit midwives into DHB positions,” she says.
She describes the workforce as like a “leaky boat”. “It might feel like you’re pouring water into the top, but it’s leaking out the bottom at the same time.”
Covid-19 may have made the situation worse, with about 10 per cent of community midwives standing down due to vaccination requirements. The Ministry of Health declined to provide figures on the extent of the impact of vaccine mandates, but says it is working with DHBs and the maternity sector “to minimise the impact of any potential temporary disruptions to maternity services caused by our response to the Covid-19 pandemic”.
And while closed borders may have slowed down immigration, Eddy is doubtful that their re-opening will solve the crisis, calling high-paying Australia a “real magnet” for a lot of midwives.
When North & South put questions to Lakes DHB, the region covering Rotorua Hospital where Lizzie Marvelly gave birth, Woman, Child and Family Service manager Jenny Martelli acknowledged in a statement that maternity services in the region were stretched, putting the issue down to the “longstanding problems” of a nationwide shortage of midwives, a lack of new graduates, and the inability for midwives from most overseas countries to be registered in New Zealand. “Contingency plans are activated immediately if there is a problem to ensure the safety of patients and staff,” she said. “Pregnant women are assured their care and the care of their babies is of high quality.” The DHB aimed to have two to three midwives on every shift, but Martelli said this was not always possible. Obstetric-trained registered nurses were sometimes appointed to help ease the pressure of midwifery shortages; there were also junior obstetric doctors “on site 24/7” and obstetricians on call; and midwives employed in management or other non-patient-contact roles were at times pulled in to provide cover, she said. The DHB was also “very appreciative” of independent lead maternity carers (LMCs) and their work. “Lakes DHB has a very active Maternity Quality and Safety Programme that is funded through the MOH and which promotes a culture of excellence in continuous quality improvement throughout the maternity service.” She said Lakes DHB welcomed feedback from whānau about their maternity services.
“All feedback, be it verbal or by way of a formal complaint, is reviewed at a weekly quality improvement meeting and then investigated thoroughly by the maternity management team.”
Officials accept there is a crisis: in April 2019, the ministry and DHBs committed to a Midwifery Accord to address staffing and workload issues, as part of a joint project with the New Zealand Nurses Organisation and the employed midwives union MERAS. The Ministry of Health says improving maternity services is a priority, and in 2020 the government allocated $242 million over four years to strengthen maternity services — the largest injection of funding to primary maternity services ever. Further initiatives announced since then include efforts to make it easier for former midwives to return to practice.
Eddy says the initiatives are good, but don’t go far enough — and evidence of concrete progress on key indicators remains thin. “We needed them five years ago, and we needed them like on steroids. We need more bigger-picture thinking and bigger levers to pull to help our workforce.”
Beneath the stories of understaffing and burnout are the hard numbers. In February last year, the Health Quality and Safety Commission’s Perinatal and Maternal Mortality Review Committee released its latest report, which covers adverse outcomes in the maternity system up to 2018.
There is some good news. Since 2007, when the committee began collecting data, perinatal deaths (those before and just after birth) have fallen markedly overall. But that’s largely where it ends. The drop in deaths came almost entirely from Pakeha mothers. Across the board, the report showed the risk of serious adverse outcomes were higher for Māori, Pacific and Indian mothers.
Other key indicators haven’t moved. From 2010 to 2018, the rate of neonatal encephalopathy has shown no significant trend up or down, as is also the case with overall mortality for newborn babies.
The committee called for a wide range of changes in response, including improving access to maternity care before 10 weeks and requiring cultural competency training across the maternity and neonatal workforce.
The government has since got to work on implementing recommendations from the committee. As of yet, it is difficult to assess whether these measures are having any impact. This year’s report from the Perinatal and Mortality Review Committee has been delayed, as have the past two annual reports from the National Maternity Monitoring Group and a report by the Health and Disability Commissioner into maternity complaints.
Leading maternity advocate Jenn Hooper says the situation feels like “Groundhog Day” — the same thing she told North & South in 2020, after being interviewed about the case of Ellie Toyoshima, who died after suffering severe, and avoidable, brain damage from being starved of oxygen during labour in 2016. Ellie was born at Hutt Hospital in a maternity unit that was understaffed and equipped with monitoring machines that weren’t working properly. She lived for just six days.
A decrease in perinatal deaths has come almost entirely from Pākehā mothers. Across the board, the report showed the risk of serious adverse outcomes were higher for Māori, Pacific and Indian mothers.
Hooper has campaigned for safety in maternity care for over a decade, co-founding Action to Improve Maternity (AIM), after her daughter Charley was born profoundly brain-damaged in 2005. In recognition of this work, she was awarded the New Zealand Order of Merit in 2019, two years after she was appointed to the Neonatal Encephalopathy Taskforce, which had a goal of reducing NE cases by 10 per cent by 2021. But Hooper is frank about the impact they’ve made. “Is there any tangible way I can show any actual changes? The truth is, I can’t.”
When the taskforce began, there were 1.19 cases of NE per 1000 live births. A year ago the rate was 1.2, says Hooper. (Official numbers are yet to be released.)
“We’ve made no impact whatsoever,” says Hooper. “It’s no surprise that we’ve made no impact because we were very, very under-resourced.”
Of late that has changed but, she says, not nearly enough to move things in any meaningful way. In Hooper’s view, the problem extends beyond staffing and resourcing to the basic design of New Zealand’s maternity system.
In 1990, the system underwent a dramatic change, as the previous doctor-led model was replaced by an autonomous midwifery model, which is unusual internationally. At the centre of this system are the lead maternity carers — mostly self-employed community midwives, who stick with women throughout the course of their pregnancy, with other services fitting in around that. The logic is that this model provides a greater continuity of care. But Hooper says it has created a system with “no real accountability”.
“We train our midwives less and trust our midwives more than in any other developed country,” she says.
In 2018, Hooper and AIM proposed to restructure the maternity sector to bring the majority of midwives within DHB employment, with a minority remaining in the community. In most cases, pregnant women would be assigned a small team by the DHB who would stay familiar with the case, while women who want to have their babies in primary care units or at home would be cared for by community midwives.
“Our idea would mean a deconstruction of the LMC system as we know it.”
The Midwives Council disagrees that such fundamental restructuring is needed.
“If you look internationally, the World Health Organization actually recommends our model of care,” says Alison Eddy. ”A midwifery-led model of care, within an integrated system that has all the pathways for referral support and extra care, is what we should be aiming for.” She says the issue is a matter of resource, and not just around recruiting more midwives.
“It’s also things like access to ultrasound in rural New Zealand for pregnant women. Having outreach obstetric clinics in high-need populations. People having access to transport.”
The organisation that represents obstetricians and gynaecologists would welcome a broader review, however.
Dr Gillian Gibson, vice-president of the Royal Australian and New Zealand College of Obstetricians and Gynaecologists, says it’s time to take a wider look at the way that maternity services are delivered in New Zealand. “To look at how we can build a collaborative system that meets women’s needs and provides equitable care and a system that people want to work in.”
She says that only by providing a strong workforce in both obstetrics and midwifery can quality maternity services be delivered in this country.
Ollie Neas is a contributing writer to North & South.
Traumatic Births: “A Club No One Wants to Join”
At the time of writing, more than two months since my daughter’s birth, I still haven’t received my discharge papers from the hospital. I was discharged hastily with high blood pressure without seeing a doctor, because they needed the bed space. I wouldn’t find out that my baby had been positioned occiput posterior (OP — the baby is face forward), which explained the unusually difficult and extremely painful labour, until my GP told me three weeks after the birth. Ellis’s OP positioning doesn’t appear to have been discovered until the surgeons pulled her out. Had we known earlier, we likely would’ve pushed for a caesarian earlier rather than attempting to wait for the induction.
After sharing what happened to me online, I was inundated with messages from parents who’d had similar experiences. I was shocked by their stories — and by their sheer number. Common themes emerged: medical professionals not listening to women and their partners, long delays in receiving treatment, dismissive attitudes minimising experiences of extreme pain, all leading to incredibly challenging beginnings for new families.
With their permission, I’m sharing some of these families’ stories.
Lydia gave birth at Auckland Hospital and was so traumatised that she and her husband have agreed they won’t ever have another child.
After a 36-week scan revealed that Lydia’s baby was in a breech position with an unusual heart rate reading, she underwent a procedure on a Sunday to turn her baby in order to undergo an early induction, scheduled to take place the next day. The procedure was successful, and the induction commenced with the routine insertion of a balloon to dilate the cervix. After more than 24 hours of intensely painful cramping, it was determined that she was ready to move to the delivery suite — but there were no beds available. She waited for another 48 hours, all the while experiencing painful contractions.
At 9:30pm on Wednesday, Lydia and her husband were finally told that there was a bed available in the delivery suite, though it wasn’t until 4am on Thursday that they were relocated. At long last, Lydia was given medication to advance her labour, and her waters broke on Thursday evening.
“I ended up pushing in the early hours of the morning on Friday and was told that they would give me two hours to push the baby out before they would medically intervene.
“After four days of physical and mental anguish, when it came to pushing I simply didn’t have the strength. After hours of trying, they tried the ventouse method before resorting to an episiotomy and forceps delivery. My little girl was finally here at 6:46am on Friday.”
While Lydia and her husband were “overcome with emotion and gratitude” that their daughter had arrived safely, they’ve since navigated a complex and difficult recovery.
“The physical recovery I knew would take time — and I really was a broken woman when I left the hospital. What I hadn’t accounted for was the mental recovery. During my three days waiting to go into the delivery suite, I think I started to go crazy. My only option was to wait and the panic about whether my daughter was okay meant I was getting desperate. I even considered calling the police at one point as it felt like I was being mentally and physically tortured.
“Once I was home, I couldn’t stop crying. I kept thinking about what had happened to me in the hospital. The waiting, the pain, the feeling of abandonment and fear for my unborn child. I could barely vocalise it to my husband or anyone really without breaking down. After several weeks I went to my doctor who confirmed I had post-natal depression which was most likely triggered by my traumatic birth experience.”
Maia’s story bears resemblances to Lydia’s. Maia gave birth at a major metropolitan hospital after what she describes as a “completely normal and pretty cruisy” pregnancy.
She went into labour at home on a Saturday night with contractions that intensified on Sunday. At lunchtime on Monday, a midwife (not Maia’s LMC, who had the weekend off) visited her, determined she had dilated only 1 centimetre and told her to rest. Maia’s support team of her mother, sister, niece, cousin and mother-in-law arrived to join her and her partner. They stayed as her contractions continued to escalate.
“When the contractions got worse we rang the midwife again. She came over checked again and I was only 2 centimetres [dilated].” She told Maia she needed to be alone and that having that many people around was not going to help. “I realise now how culturally insensitive that comment was.”
Not long after the midwife left, Maia’s pain worsened significantly. “My mum rang the midwife again and she basically told my mum she was overreacting. That really pissed Mum off — after birthing four children including twins she felt she had some knowledge of birth — and she told the midwife we were going to hospital even if she didn’t agree.”
She says no one took responsibility for her, and when she did finally see a midwife, she was offered pethidine to help with the pain. She had concerns about taking pethidine, preferring an epidural, but as it was the only option offered to her she consented to a low dose.
“At about 4am the contractions returned and Mum went looking for a midwife to help because no one had come to check on me since midnight. She found them sitting around yarning and when she asked them they were rude and told her they’d be there shortly. She was then checked again and her dilation was 5 centimetres. Maia was told she could have an epidural, which she consented to. She received the epidural at 10am on Tuesday, the wait due to only one anaesthetist being on duty. It did not bring the relief she hoped.
“Basically, it didn’t work. The worst thing is I felt them putting in the catheter — I can’t describe how horrible that felt. They tried a second epidural but it still didn’t work.
“I remember from this point on feeling like I had completely lost control of my body. I had been poked and prodded and naked in front of so many people that this was no longer my own experience. I just wrapped my arms around my knees and zoned completely out, like I wasn’t there anymore, in this nightmare.”
It wasn’t until the arrival of the unit’s head midwife, who was also a family friend, that Maia finally received the care she needed. “Our family friend arrived around 12pm and decided straight away that I needed to have a C-section and get the baby out. My partner and I went into theatre five minutes later and they attempted a spinal but that didn’t work either, so they put me to sleep and my partner had to leave.
“I woke up and my partner asked if I wanted to hold my son, and I said no. I was so out of it and exhausted I just couldn’t. I don’t actually remember the first time I held him.”
Later, hospital staff would acknowledge that mistakes had been made. “Someone came into my hospital room after the birth and apologised for not taking my pain seriously. They realised the cord was short and so every time I had a contraction, it would pull the placenta.
“I feel like there were undertones of racism. One thing I have realised is that I suppressed how bad the pain was because I’m Māori and I’ve subconsciously learnt to act a particular way in certain settings . . . I wish I’d had a Māori LMC. I met one not long after giving birth and I remember thinking, ‘She would have advocated for me’.”
Maia and her partner are also reluctant to have another child. “For a long time I laughed off how horrendous my son’s birth was — until about a year later, I was on a girls’ trip with friends and half of them were pregnant with their second baby and I thought, ‘Wow, I have no desire to have another baby.’ In fact the idea makes me feel sick. Basically I broke down, realising how much the birth had affected me.
“I went to counselling and found out I had post-traumatic stress disorder. I still don’t want to have another baby and maybe I never will, but I still feel pressure to, from just life and society. My partner jokes sometimes but he understands. He was there.”
Another new mum, Rachel*, also ended up needing a C-section after a long and protracted birth made worse by an understaffed regional hospital. The hospital’s staffing issues became apparent as soon as Rachel arrived.
“When I arrived at the hospital I was brought into a birthing room and quickly realised the room wasn’t equipped, as the staff had none of the supplies they seemed to need. This was just one small problem that became apparent during my labour.”
Rachel’s LMC determined that she needed continuous monitoring to check the wellbeing of her and her baby, as she was experiencing unexpected symptoms.
“A staff member at the hospital did what they could to support and monitor me, however the medical complications were being dismissed by the doctors on duty and they were busy with other women that they needed to attend to due to low staff.”
Rachel and her partner’s concerns for their baby’s wellbeing intensified as the hours wore on.
“The afternoon following our admission to hospital we discussed the option of a caesarean section with the medical team, as we knew in our gut it was the safest option for myself and our child. We were told to wait until morning. It came across as if they just didn’t have the staff to support this medical intervention at that time.”
During the night, Rachel’s condition worsened. “My contractions were getting much longer than they should be and at times were relentless without even 30 seconds’ rest between. Blood gushed from me with every contraction, making me incredibly nervous for the health of our baby.
“All throughout this experience my support person and I were alone, except for the semi-routine checks by the night nurse. By the morning I was exhausted, in pain and only 4 centimetres dilated.
“Eventually, with much advocating by my partner, the doctors agreed and called an emergency caesarean to deliver our baby. At that moment I felt defeated. I couldn’t help but feel if other steps had been taken earlier and more support would have been available the birth of our baby could have looked so different.”
Another emergency caesarean delivery, this time after a labour more than 60 hours long, marked the beginning of parenthood for Victoria*.
“I don’t know what I expected when I gave birth but it certainly wasn’t what actually happened to me. I didn’t expect a Hollywood ‘waters breaking, sweaty screaming’ situation but what actually happened feels like a story from the 1800s rather than 2019.
“My birth story ends happily and both my daughter and I are healthy. This is a sentence I hold on to sometimes whenever I start to replay events in my brain.”
Victoria went into labour 11 days before her due date, and was admitted to Auckland Hospital after almost 12 hours in labour at home. When she reached the hospital, she felt optimistic, breathing deeply and feeling that each contraction was bringing her closer to meeting her baby. As it transpired, it would be another 50 hours before that happened — another heart-rending story of mismanaged pain, an exhausted mother labouring for hours with no result.
“I pushed for so long that our midwife had to take a break to lie down and my wife took over. We held the end of a towel each as I pushed through each contraction. I must have pushed for more than 4 hours and was exhausted.
“I was told that I had all the pain relief available despite the epidural not working. Everyone was kind and supportive but no one was in my corner fighting for me. No one was looking at the woman on the table, fully dilated, making no progress. No one was moving the heart monitor tabs on a baby, who could have moved during labour.
“Eventually, despite being scanned and examined by senior staff and our midwife, the team realised our baby was in the occiput posterior (OP) position meaning she was trying to come out face first with her spine against mine. It is really uncommon for babies to remain in this position and it is incredibly hard for first-time mothers to deliver without intervention. I was rushed into an emergency caesarean and our daughter was born within 15 minutes.”
The pain didn’t end there: Victoria’s daughter had lost weight and had problems attaching for feeding, which led to ongoing issues for 12 weeks.
“No one in the healthcare profession once thought to talk us through potential issues with a long labour or an OP birth,” Victoria said. “Babies kept in that position can suffer distress, spinal cord damage, permanent brain damage or death. None of this was ever discussed with us either prior to giving birth, during or afterwards. Our daughter was in pain with a locked jaw for weeks because of a long delivery and the main focus of any healthcare professional was whether I could breastfeed her.”
Birth-related problems didn’t stop. “Two years later, I was admitted to A&E with extreme back pain, which they believe is due to a fractured pelvis most likely incurred during labour. The consequences of labour are not something ever discussed pre- or postpartum with women and leaves lots of people isolated and struggling with injuries or mental health issues that can take months or years to remedy. The system also fails to support partners who, after experiencing watching their partner give birth, are often left with traumas of their own.”
Stories like these are heartbreaking, personal, and share similarities that expose a system under catastrophic stress.
When I went to see my GP three weeks after the birth, she agreed that I was experiencing post-traumatic stress disorder. As we filled out the ACC claim form for support during my recovery she gave me a look of sad resignation. “Prepare yourself for them to decline your claim,” she said. With so many women having similar experiences, ACC may well view my horror story as normal.
There should be nothing normal about what happened to me, Lydia, Maia, Rachel and Victoria. And I wonder just how many Kiwi families are being let down by our hospitals. As so many women suffer in silence, I expect the scale of the problem could never be properly understood without a nationwide formal inquiry.
With the planned reorganisation of the health system from the district health board model to a centralised mode of delivery, an inquiry would be timely lest the new system perpetuate the mistakes of the old. Questions top of my mind are whether new guidelines should be established to limit the time that birthing parents labour or experience excessive pain without significant progress before interventions are proactively offered, whether information about the complexities of OP births should be included in the antenatal curriculum, and whether ultrasound scanning should be used routinely during protracted labours to establish any concerns about positioning. Experts would no doubt have other suggestions.
It is absolutely clear to me that our health system is dangerously under-resourced, a situation that makes traumatic and tragic outcomes all the more likely.
No investigation or inquiry will give back to traumatised families the birth stories they were meant to have. But if it prevents even one woman going through what Lydia, Maia, Rachel, Victoria and so many others went through, it will be worth it.
Our babies deserve better. We deserve better.
Lizzie Marvelly lives in Rotorua. She is a writer and has worked professionally as both a classical and contemporary singer.
This story appeared in the May 2022 issue of North & South.
